What is sterilisation?
Sterilization is a widespread and accepted method of contraception and intended to be permanent. However, approximately 5% of women regret their decision. In general, the younger the woman is at the time of sterilization, the more likely she is to regret her decision. Reasons for requesting sterilization reversal include: partner change or remarriage, wanting more children, death of a child, changes in attitude or mental health.
What are the options available for women who had been sterilized and wish to conceive?
The two options are: reversal of sterilization and IVF. Both are not usually available on the NHS in the UK and health insurance rarely pays for it. Furthermore, the insurance coverage varies widely among various insurance companies.
There is a need for well-designed controlled clinical trials to compare the efficacy and safety of reversal and IVF in restoring fertility in women seeking pregnancy following tubal sterilization.
What is reversal of sterilization?
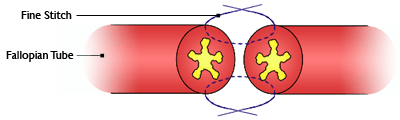
In sterilization the fallopian tubes are tied, cut or blocked so that eggs cannot be transported into the womb where they might be fertilized. Sterilization reversal aims to reconnect the fallopian tubes if they are not badly damaged.
The operation is done under a general anaesthetic through a bikini incision (laparotomy). The ends of the tubes are trimmed to remove damaged tissue and reconnected using very fine sutures. The operation is done using an operating microscope (micro-surgery). Most women will need to be in the hospital for approximately 3 days. In some patients, the procedure may be performed using a keyhole surgery (laparoscopy). To date, no large studies have compared the efficacy and safety of laparotomy versus laparoscopy for reversal of sterilization.
What are the issues that need to be considered before making a decision?
A number of pertinent issues should be considered:
- The quality and quantity of husband/male partner sperm. If the sperm quality is poor then IVF+ ICSI is a better option than reversal
- Sterilization method:
- The longer the length of the fallopian tube after reconnecting its ends, the better the chance for pregnancy.
- A review of female sterilization reversal studies found that live-birth rates varied according to occlusion techniques: ~40% after reversal of electrocoagulation (tube burnt), ~50% after reversal of the Pomeroy procedure (tubal ligation), ~75% after reversal of rings, and ~85% after reversal of Filshi clips.
- The condition of the fimbria of the tubes is also important as well as the presence of adhesions (scar tissue) and endometriosis - in these conditions IVF is a better option.
- Time to conceive: The cumulative pregnancy rates at 6, 12, 18 and 24 months following reversal of sterilization were 43%, 64%, 68% and 72% respectively. Of the pregnancies 56% were achieved within 6 months and 83% after 1 year (Gordis et al 2007 ESHRE).
Both IVF and sterilization reversal are generally not recommended for women aged 42 or older and for women who have reduced ovarian reserve (a decline in either egg quantity or quality earlier in life than expected). IVF with donated eggs is a viable option in these circumstances.
What are the pros and cons of reversal and IVF?
| Reversal of sterilization | IVF and embryo transfer | |
| Procedure | Major surgery to reconnect tubes | Ovarian stimulation, egg collection and embryo transfer |
| Pregnancy | Natural conception | Medically assisted |
| Multiple pregnancy | 1% | 25% |
| Ovarian hyperstimulation syndrome | 0% | 5% |
| Cost | $10000-25000 (USA) £ 3000-4000 (UK pound) |
$10000-30000 (USA) £3000-4000 (UK pound) |
| Success rates | 50-70% per year | 20-40% per treatment cycle |
| Length of time to know outcome | A year or more | Two weeks after embryo transfer |
| Ectopic pregnancy | 10% | 1-2% |
| Future contraception | Family planning may be needed | No |