What causes miscarriage?
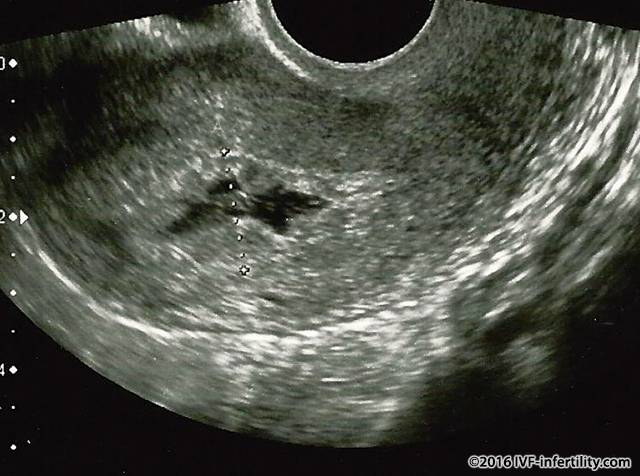
Ultrasound image of incomplete miscarriage
There are several causes of miscarriage that have been identified. These include chromosomal abnormalities, gene defects, hormonal problems, infection, immunological, uterine abnormalities, chronic maternal illness and environmental hazards. In a significant proportion of women the cause of the pregnancy loss remains unexplained after careful investigation.
Chromosomal abnormalities
Fetal chromosomal abnormalities are the commonest cause of sporadic miscarriage affecting more than half of all early miscarriages. In couples with recurrent miscarriage, chromosomal abnormalities of the embryo account for 3%. The risk of miscarriage resulting from chromosomal abnormalities of the embryo increases with advancing maternal age. Chromosomal abnormalities may be due to abnormalities in the egg, sperm or both. The usual chromosomal pattern is 46 chromosomes which are arranged in 23 pairs, one of these pairs is called sex chromosomes, females will have two X chromosomes and males will have one X chromosome and a Y chromosome. The genes we all have are lined up along the chromosomes. For each of these genes there are two copies. A person will inherit one copy of each gene and one of each pair of chromosome from each parent. There are two types of chromosomal defects: numerical and structural. The most common chromosomal defects are:
Trisomy
A trisomy is where there are three chromosomes of one type instead
of the normal pair. The resulting embryo will then have 47 chromosomes
and will either abort, or produce a baby with congenital abnormalities.
Trisomy constitutes the largest group and is more common as maternal age
increases. These faults are not very likely to recur and there is a good
chance that the pregnancy will be right next time.
Monosomy
A monosomy is where there is one chromosome missing. Only 1% of pregnancies
with one X chromosome will survive and the condition is called Turner's
syndrome.
Polyploidy
A polyploidy is where one or more extra complete set of chromosomes
are present, this may be the result of an egg being fertilized with more
than one sperm.
Unbalanced translocation
This is a less common cause of miscarriage. Some of these abnormalities
are inherited from one or another of the parents who has what is called
balanced translocation where one of the chromosome swapped bits of its
genetic material with that of another chromosome. Approximately 3% of couples with recurrent miscarriage, one of the partners carries a balanced
structural chromosomal anomaly, this usually causes
no problem to the parent as all his or her genetic materials is present,
it is just some of it is in unusual place. There would be a significant
risk of a fetus inheriting what is called unbalanced form of this translocation,
which may means the fetus would have either too much or too little genetic
material. This situation may cause fetal death and miscarriage or fetal
abnormalities.
Gene defects
Some gene defects may cause miscarriage, but most results in a more serious problem with the baby such as cystic fibrosis or Duchenne muscular dystrophy.
Hormonal problems
Several different problems may fall in this category including low progesterone levels, high LH levels, or thyroid abnormalities.
Low progesterone level
If too little progesterone is produced by the corpus luteum, the endometrium
may not develop adequately to sustain the pregnancy. However, low progesterone
levels in early pregnancy usually reflects a pregnancy that has already
failed.
High LH levels
Elevated levels of luteinizing hormone is common in women with PCOS.
High LH affects the quality of the eggs and hence the embryos, and may
result in recurrent early miscarriages.
Thyroid abnormalities
Thyroid abnormalities may also cause miscarriage. Thangaratinam and colleague reported positive association between thyroid antibodies and miscarriage and preterm births even when the thyroids are functioning normally (BMJ 2011).
Infection
Any severe infection such as rubella, cytomegalovirus and listeria can cause sporadic miscarriage. Bacterial vaginosis also can cause late miscarriage, preterm labour and premature rupture of membranes. The role of infection in recurrent miscarriage is unclear.
Immunological
- Antiphospholipid antibodies syndrome (APAS) is present in about 15% of women with recurrent miscarriage (compared with 2% normally). These antibodies circulate in the blood and can cause thrombosis of the placental vessels, and if this happen, the baby dies. The association between APAS and miscarriage is stronger for second trimester losses than for the first trimester losses.
- Inherited thrombophilic defects including factor V Leiden mutation, deficiencies of protein C and protein S and antithrombin III, hyperhomocysteinaemia and prothrombin gene mutation have been implicated as a possible cause in recurrent miscarriage and late pregnancy complications. The association between thrombophilia and late pregnancy loss has been consistently stronger than for early pregnancy loss.
- Excess or hyperactive Natural Killer cells. NK cells are subset of the immune cells and are subtyped by the expression of CD56 and CD16 surface antigens. The majority of the blood NK cells exhibit CD16 but have fewer CD16 and are responsible for destruction of foreign antigens. Uterine NKC reside in the uterus and express the CD56 antgen on its surface. Uterine NK cells release a variety cytokines, which are important in endometrial receptivity and vascularisation. However, excess or hyperactive uterine NK cells can damage the cells which make the placenta as well as the endocrine system that produce hormones essential for pregnancy. The cause of excess or hyperactive NK cells is unknown.
- The couple’s A pregnancy is recognised as a foreign because the father HLA (group of cell surface molucles which are encoded by major histocompatibility gene) is different from that of the mother. The mother makes blocking antibodies that attach to and camouflage the placenta (protecting antibodies) If the father‘s HLA is too similar to that of the mother, The embryo will not be protected because it will not be able to differentiate itself from that of the mother, leading to lack of developing blocking antibodies and the pregnancy fail too early for tissue to pass.
- TH1:TH2 Cytokine ratio Cytokines are chemical messengers in the blood. High levels of the TH1 pro-inflammatory cytokine, TNF-alpha, in particular, have been shown to be associated with reduced egg quality, implantation failure and miscarriage.
- Antibodies to the baby DNA or DNA breakdown products such as ANA.
- Antinuclear Antibodies (ANA), Anti-Histone and ds-DNA antibodies.
Uterine abnormalities
There are several uterine problems that may result in miscarriages. These include a misshapen uterus, fibroids, cervical impotence and adhesions.
Mis-shapen uterus
Some women with abnormally shaped uterus miscarry. The reason for this
is not fully understood but it is possible that the uterus may not enlarge
enough to accommodate the pregnancy. The miscarriage often occurs in the
second trimester, but early losses may occur as well. Uterine abnormalities
are present from birth and include a septate uterus (a uterus divided
by a wall) and double uterus.
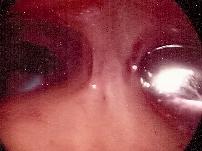
Fibroids
Fibroids sometimes distort the uterine cavity and prevent pregnancy from
implanting properly.
Cervical incompetence
During pregnancy, the cervix (neck of the womb) should remain closed
until labor begins. In some women, the cervix is weak and starts to open
up quite painlessly with subsequent spontaneous rupture of membranes and
expulsion of the fetus. Miscarriage caused by cervical incompetence
is usually late in pregnancy, often after 16 weeks. This weakness of the
cervix may be an inborn fault, cervical weakness is frequently associated with uterine
malformation. Other causes include a previous surgery such
as many D&C procedures, and LLETZ (large loop excision of the transformation zone) for removal of cervical abnormal cells.
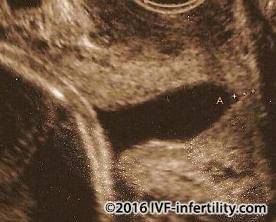
Adhesions
Adhesions inside the womb cavity (Asherman's syndrome) may not only
cause infertility but may also be associated with miscarriage possibly
by restricting the implantation and growth of the fetus.
Endometrial causes
Miscarriages may be associated with retarded endometrial development
(luteal phase defect).
Chronic maternal illness
Some chronic diseases in the mother such as diabetes mellitus, very high blood pressure, kidney problems, systemic lupus may occasionally cause miscarriage. However, with all these diseases, normal pregnancy is the usual.
Environmental hazards
Any substance that result in toxicity in a pregnant woman may be implicated in miscarriage including, radiation, some insecticides, lead, toxic chemicals. Cigarette smoking, alcohol and caffeine consumption have been associated with an increased risk of spontaneous miscarriage in a dose-dependent manner.