Semen analysis
The semen analysis test is the most important infertility test. Semen analysis is the first step in the medical evaluation of male infertility. The semen analysis test is usually performed after 3-5 days of sexual abstinence. The clinic usually provides the man with written instructions about the method of collection. The sample is usually collected after masturbation into a sterile pot. The volume of the ejaculate is measured, and liquefaction of the ejaculate is estimated. Then a drop of semen is examined under the microscope where the number of sperm is counted, how they move around is assessed, and the proportion of normal sperm can be estimated. Semen assessment should be performed in accordance with World Health Organization (WHO) methodology. The WHO semen values are based on populations of fertile men and are described as 'reference' values rather than 'normal' values.
You may be asked to produce a “split-ejaculate” collecting the first one or two spurts of the ejaculate into the “first pot” and the remainder into the “second pot”. The reason for the split ejaculate is to assess each pot separately. Pot one usually contains the best sperm.
Providing a semen sample by masturbation can be very stressful for some men. Men who have this problem should ask for help, their wives can help them to provide the sample, other methods such as mechanical vibrators, viagra tablet can help some men to get an erection. If all this fail it is possible to collect semen sample using a special condom during sexual intercourse.
Normal values of semen variables (WHO 2010):
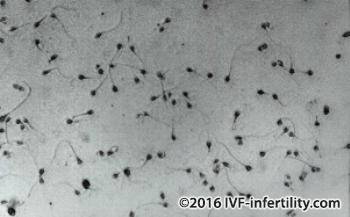
Volume: 1.5 ml or more.
Liquefaction: normal (immediately after ejaculation the semen contains jelly like particles but after about 30 minutes these should liquefy more or less completely).
Count: 15 million or more sperm per ml.
Morphology: 4% or more of the sperm should have normal shape.
Motility: 40% more of the sperm should be swimming. Progressive motility (moving forward) 32%.
Vitality (live): 58% or more of the sperm should be alive.
Cells: white cell count should be less than 1 million per ml. If there are more cells, this may be an indication of an infection.
It is well known that the results of semen analysis can vary between different men as well as between different ejaculates from the same man. A normal sperm test is reassuring.Remember that fertile men may have from time to time an abnormal test, so a single abnormal semen analysis test is of little significance. However, if the test is abnormal the test will need to be repeated two to three times over two to three months to confirm whether the abnormality is persistent or not.However, if a gross sperm deficiency has been detected the repeat test should be undertaken as soon as possible,
It is just not possible to say with certainty that a man with a low sperm count is infertile, as many men with low or moderately low sperm counts are fertile. Similarly, it is not possible to say with certainty that a man with a normal count is fertile as his sperm may be lacking fertilizing capacity.
Normozoospermia when all semen parameters are normal.
Azoospermia is defined by absence of sperm in the ejaculate.
Oligospermia is defined by low sperm count.
Cryptozoospermia is defined as absent sperm from fresh semen preparations but observed in a centrifuged pellet due to very low sperm count.
Asthenospermia is defined by low sperm motility.
Teratozoospermia is defined by high proportion of abnormal sperm in the ejaculate.
Aspermia - no ejaculate
Necrozoospermia- all sperms are non viable